- About
- Contact
- Introduction to Urinalysis
- Abnormal Urine Volumes
- Urine Specimen Types, Urine Collection, Specimen Preservation
- EXAMINATIONS OF THE URINE AND TESTS FOR
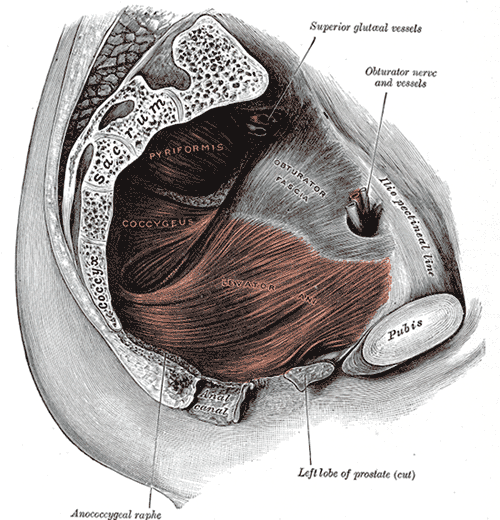
- ANATOMY AND PHYSIOLOGY OF THE URINARY TRACT
- Urine Chemistry and Pathophysiology
- PATHOPHYSIOLOGY OF DISEASES OF THE URINARY TRACT
- BACTERIAL INFECTIONS
- FUNGAL INFECTIONS
- PARASITE INFECTIONS
- VIRAL INFECTIONS
- Synovial and Joint Fluid
- Cerebral Spinal Fluid (CSF)
- Pericardial Fluid
- Peritoneal Fluid
- Pleural Fluid
- Amniotic Fluid
- References
- Automated Urinalysis
Urinary Tract Infection (UTI):
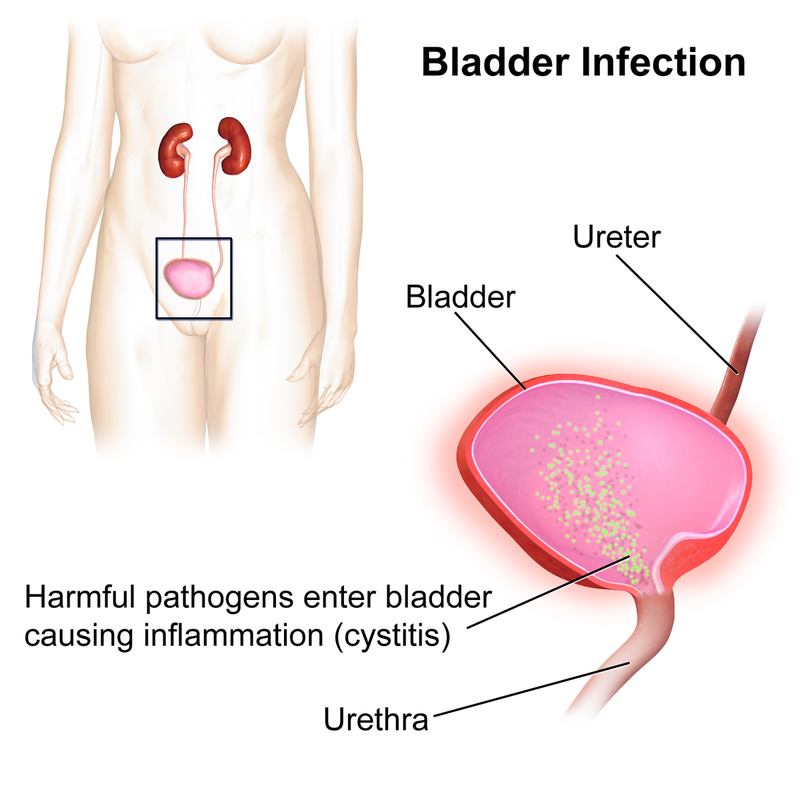
Bladder Infection (Cystitis)
- Inflammation of the bladder and/or urethra (lower UTI)
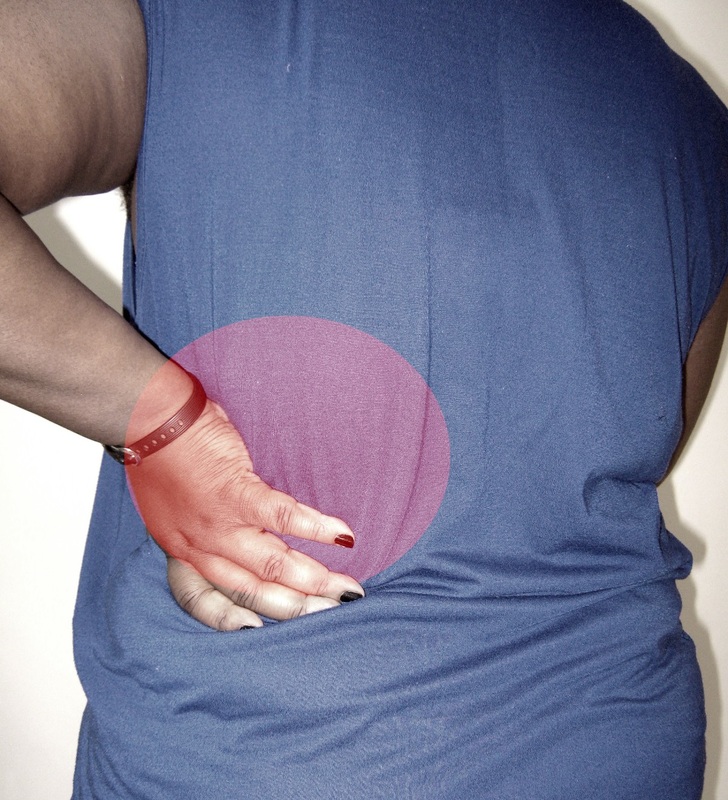
- Symptoms: urgency, frequency, incontinence, pelvic pain and pressure, low back pain, bladder spasm, fever, chills, burning, dark yellow urine, or pink-to-red urine if blood is present (hematuria)
- Bacteria may travel through the urinary tract up to the kidney and cause a kidney infection called pyelonephritis
- Cause: usually bacteria (Enterobacteriaceae: E. coli, Klebsiella, Enterobacter, Proteus, Pseudomonas), STDs, yeast, viruses, parasites, chemotherapy or radiation, catheterization
- Treatment: antibiotics, fluid, rest
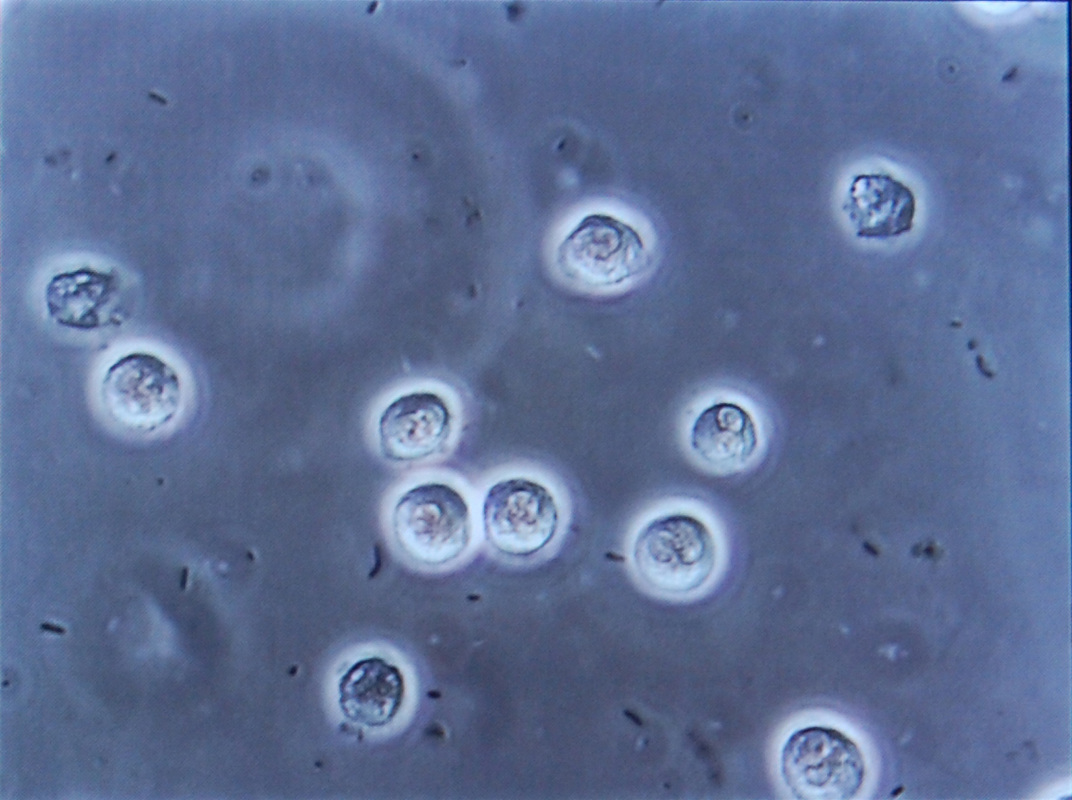
Pyuria:
- Urine contains white blood cells and/or pus (exudate), which is a combination of dead bacteria and dead white blood cells and cellular debris
- Sign of inflammation
- Rich in protein
- Foul-smelling
- Greenish-yellow
- 6-10 or more polymorphonuclear neutrophils/hpf (microscope) in mid-stream, clean catch, voided urine that has not been spun down
- Typically a sign of a bacterial urinary tract infection (UTI)
- May also occur with STD's, such as gonorrhea or viruses
- Patients with sepsis may have pyuria
- Patients with pneumonia may have pyuria
- Patients with pyelonephritis, a bacterial kidney infection, may have pyuria, flank (side) pain, tenderness, fever, nausea, painful urination, frequency, loss of appetite, vomiting, malaise, weight loss, blood in the urine (hematuria)
- Close watch must be kept on this condition, which can rapidly lead to a buildup of pus surrounding the kidney, sepsis, or even cause the kidneys to go into kidney failure if left untreated
- Usually starts out as a bladder infection, cystitis, or prostatitis
- Those over age 65 are at higher risk for complications, and the risk of death from pyelonephritis and sepsis is around 40%
- The most common cause is the bacterium Escherichia coli
- Close watch must be kept on this condition, which can rapidly lead to a buildup of pus surrounding the kidney, sepsis, or even cause the kidneys to go into kidney failure if left untreated
- Occasionally associated with drugs such as acetaminophen
- Risk factors: frequent UTI's, STD, sexual intercourse, diabetes, use of spermicide, other forms of birth control, structural anomalies of the urinary tract
- Urinalysis and urine culture are laboratory tests which aid in the diagnosis and treatment of this condition
Urosepsis:
- Septic shock signs include rapid breathing, shallow breathing, pallor, rapid heart beat, low blood pressure, shivering, confusion
|
|
Pyelonephritis (Kidney Infection)
- Pyelonephritis is the most common type of renal disease
- Nosocomial (hospital-acquired)
- Usually caused by coliform bacteria or enterococci that enter the urinary tract
- Often catheter-associated
- E. coli most common cause
- Klebsiella spp
- Pseudomonas spp
- Usually caused by coliform bacteria or enterococci that enter the urinary tract
- Community-acquired
- Usually caused by coliform bacteria that inadvertently enter the urinary tract:
- E. coli (70-80%)
- Enterococcus faecalis
- E. coli (70-80%)
- Usually caused by coliform bacteria that inadvertently enter the urinary tract:
- Nosocomial (hospital-acquired)
- Inflammation of the renal pelvis and connective tissue of the kidney or kidneys
- Usually due to bacterial infection (UTI) where bacteria has traveled from the bladder to the kidney or kidneys and usually starts out as a bladder infection, cystitis, or prostatitis
- Bacteria travels to the kidney and creates biofilms that may be antibiotic-resistant
- Pregnancy may be a cause of this as well
- Renal calculi (stones) may also cause it
- Benign prostatic hypertrophy may also cause (enlarged prostate) in males
- Structural anomalies may cause it or cause one to become more prone to developing it:
- Reflux (urine flows back into the bladder)
- Stones or strictures blocking the ureters or urethra
- Urinary stents
- Urinary catheters
- Shortened or angled urethra
- Drainages
- Urogenic bladder
- Pregnancy
- Medications
- MS
- Spina bifida
- Spinal injuries
- Prostate diseases
- Diabetes mellitus
- Immunocompromisation
- Sexual intercourse
- STD
- Spermicide use
- Reflux (urine flows back into the bladder)
- Pus builds up in the renal pelvis, and sometimes includes abscesses
- Symptoms: rapid onset of fever, aches, chills, nausea, vomiting, flank (side) and low back pain, often following a UTI (urinary frequency and urgency), foul odor to the urine, pyuria, hematuria, tenderness
- If it progresses to septic shock, see symptoms under "urosepsis" above
- Risk factors: underlying UTI, kidney stone, enlarged prostate, pregnancy, tumor, women affected more often, sexual activity, poor hygiene, catheterization
- Diagnosis: clean-catch urine (urinalysis) with increased RBCs, WBCs, pus, protein, casts, and nitrite (bacteria)
- Treatment: antibiotics, fluids, rest, correction of underlying causes, which may include surgery to remove an obstruction
Polyuria: Increase in Urinary Frequency
Polydipsia: Increase in Thirst, Associated With Diabetes
Glomerulonephritis (Kidney Infection: Autoimmune)
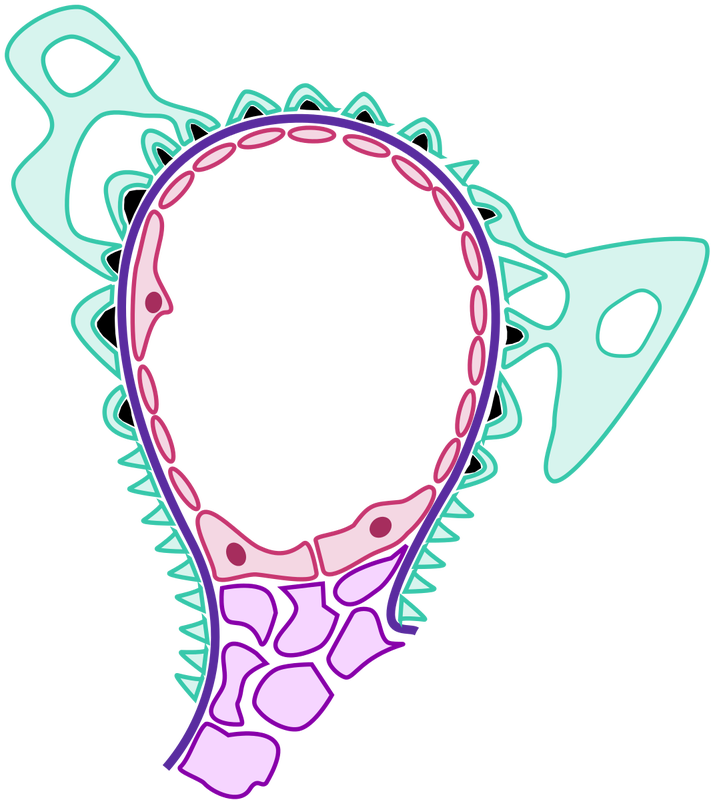
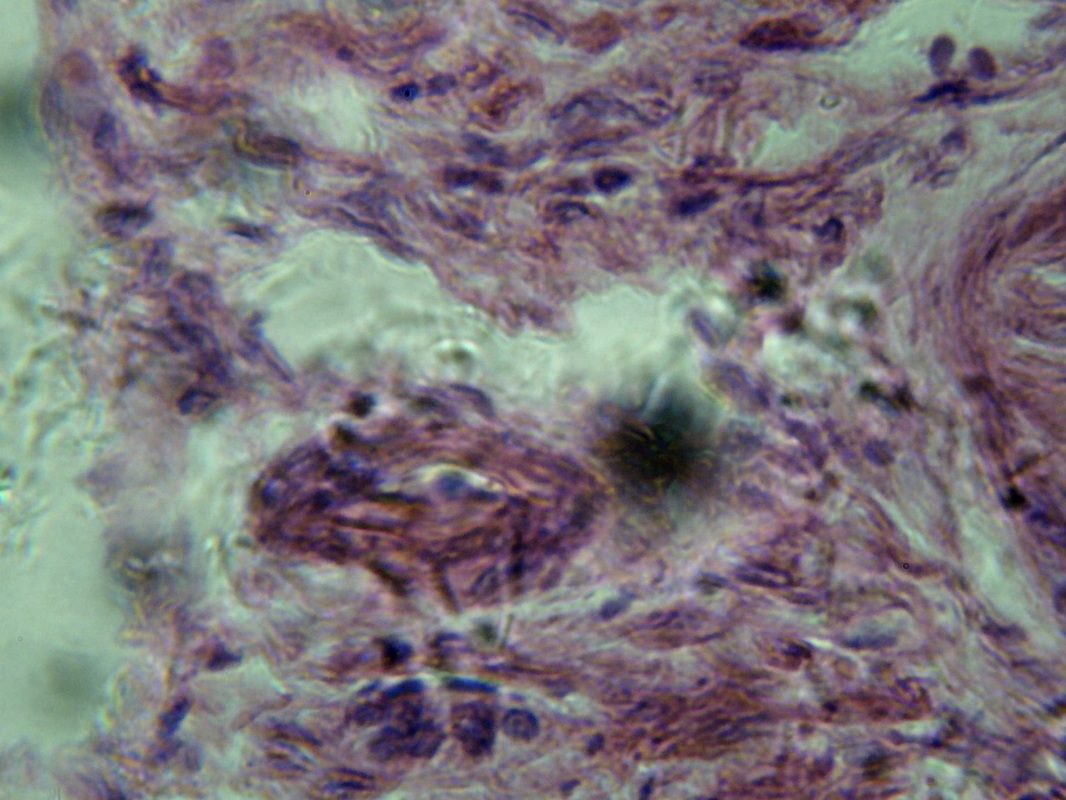
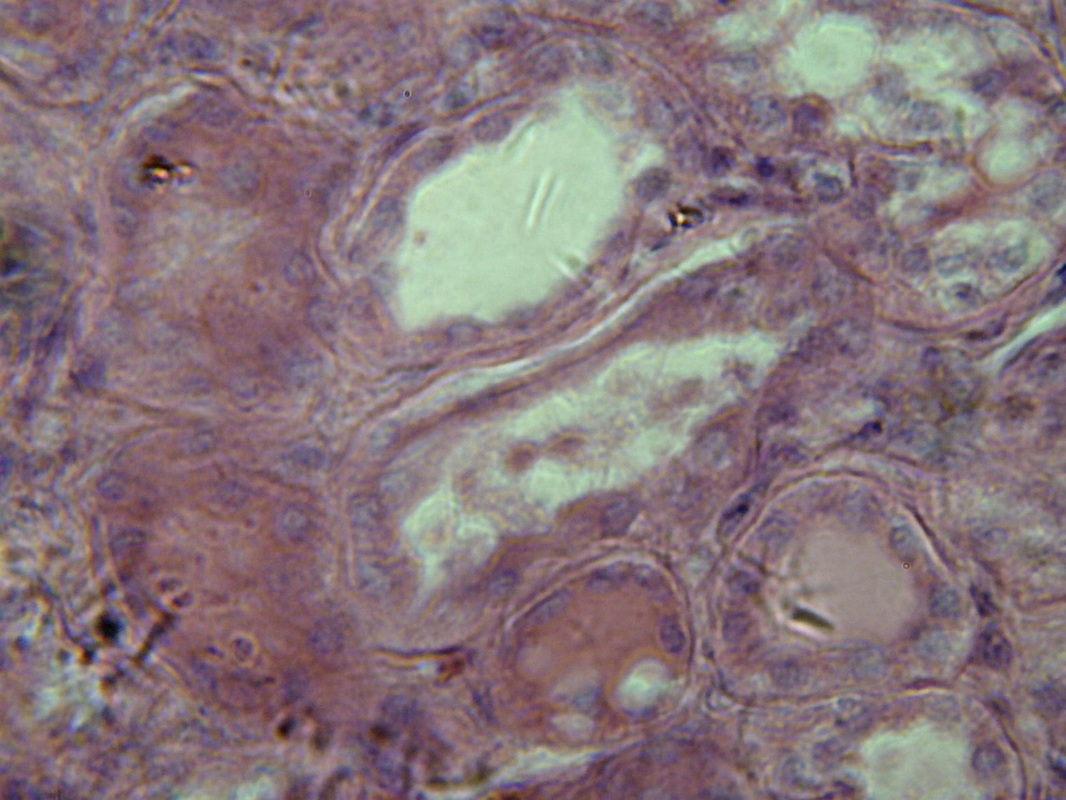
- Acute Glomerulonephritis: inflammation and swelling of the glomeruli of the kidneys (1)
- Primary Glomerulonephritis
- May or may not have a specific cause
- May result from an autoimmune disease that causes circulating antigen-antibody complexes (large) that get stuck in the capillaries of the glomeruli
- Tumors can cause this
- Cysts can cause this
- Autoimmune diseases like lupus can cause this
- Secondary Glomerulonephritis
- Due to some other systemic disease, such as a bacterial infection such as streptococcal bacterial infection of the throat or skin that went unnoticed or untreated
- Children, teens and young adults are affected more so than older adults, as it usually follows Strep Throat (bacterial infection) 1-2 weeks later
- Streptococcus pyogenes (Group A strep) is usually the cause
- Usually resolves in 2 weeks and results in recovery
- Some cases may result in long-term disease/damage as seen above under primary glomerulonephritis
- Results/consequences include:
- Decrease in glomeruli filtration rate
- Water and salt retention in the body
- Signs and symptoms include the following:
- Blood in the urine (may be obvious or subtle; urine may appear dark or coffee-colored)
- Detected by urinalysis, and includes presence of RBCs, WBCs, renal tubular cells, casts
- Protein in the urine
- This is due to the increased permeability of the glomerular membrane, and protein in the urine is typically not normal
- Elevated blood urea nitrogen (BUN)
- Elevated erythrocyte sedimentation rate (ESR)
- Hypoalbuminemia
- Kidneys may be swollen/enlarged on radiographic film
- Edema (swelling/puffiness)
- Decrease in urine volume
- Raised blood pressure
- Headaches
- Visual disturbances in some cases
- Malaise
- Loss of appetite
- Low-grade fever
- Low back and/or flank (side) pain
- Blood in the urine (may be obvious or subtle; urine may appear dark or coffee-colored)
- Treatment:
- Unfortunately, there is currently no treatment for the poststreptococcal glomerulonephritis except antibiotic therapy for the infection if it is still present
- Diuretics: these can be given to aid in controlling swelling and edema and high blood pressure
- Restriction of sodium intake
- Corticosteroids to prevent immune reaction are the only therapy available for autoimmune types of glomerulonephritis
- Chronic Glomerulonephritis:
- Slow and progressive
- Noninfectious
- May lead to irreversible renal damage and even renal failure
- An advanced stage of kidney disorder
- Inflammation and destruction of the glomeruli of the kidneys, leading to reduction in GFR
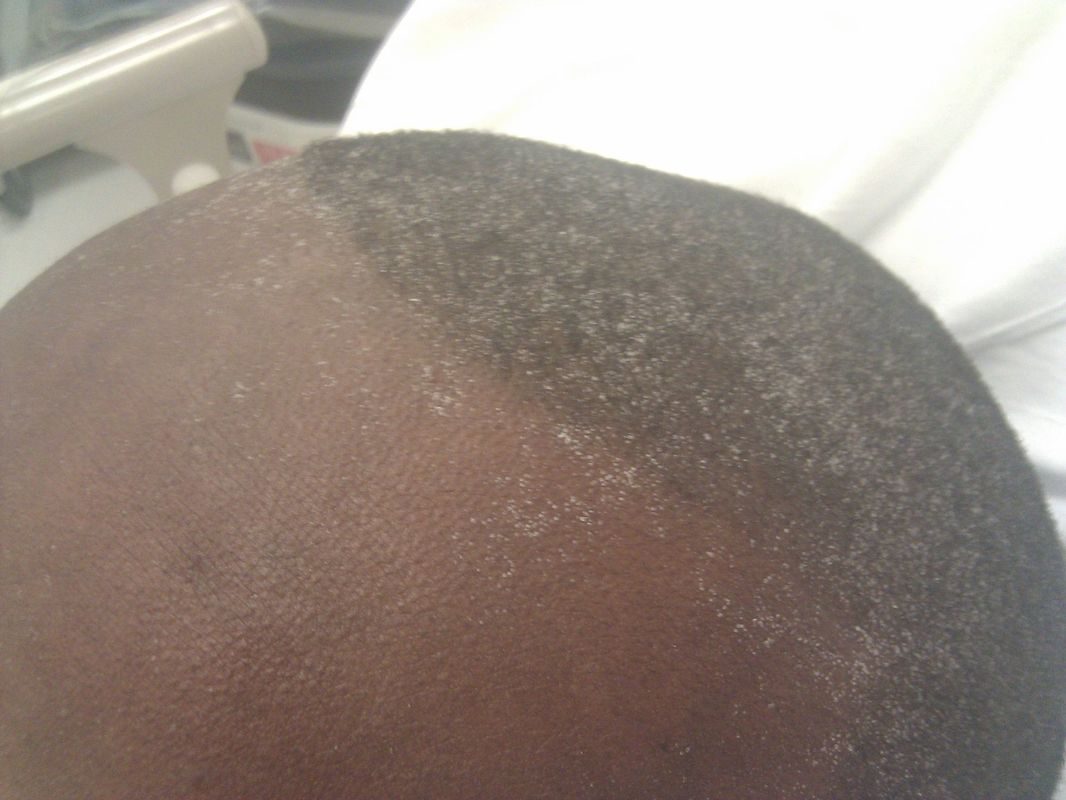
- Gradually leads to high blood pressure, blood in the urine, protein in the urine, edema and swelling, oliguria (decreased urine production), excess urea in the blood (azotemia) resulting in crystals of urea on the skin (uremic frost), fatigue, malaise, nausea, vomiting, itching, shortness of breath
- Treatment for chronic glomerulonephritis:
- Diuretics, antihypertensives, antibiotics if UTI exists, restriction of protein and salt, ACE inhibitor, and dialysis, if required, possible kidney transplant
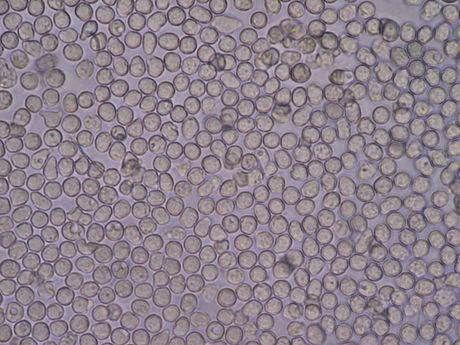
Hematuria: One of the Symptoms of Acute Glomerulonephritis
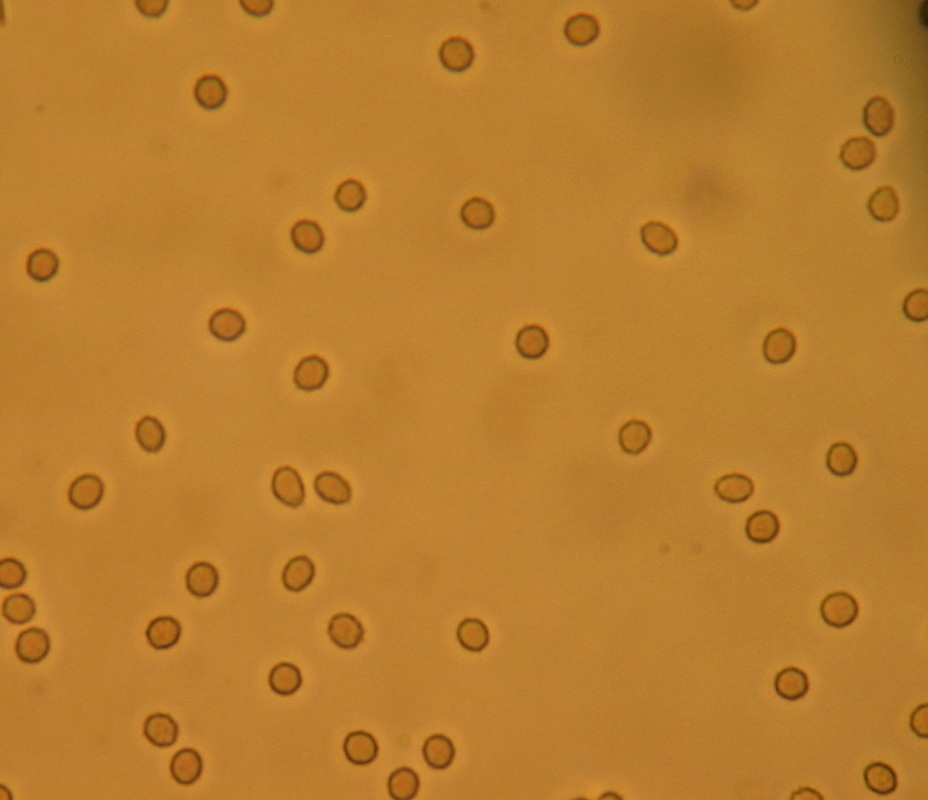
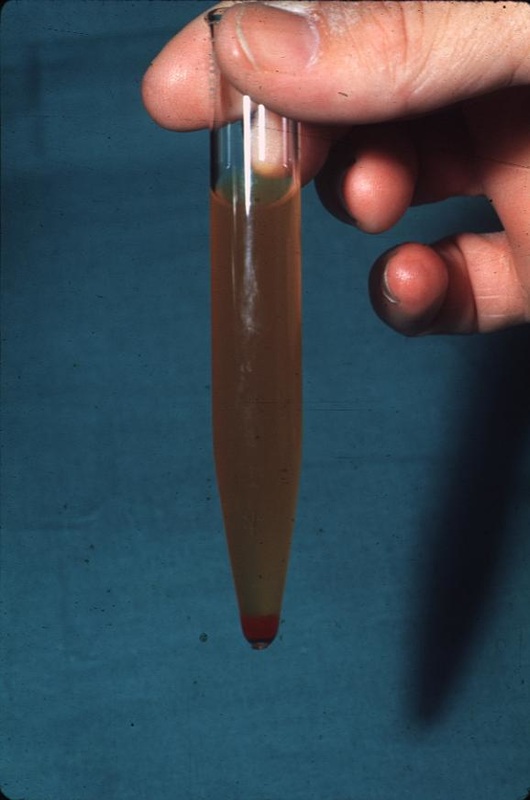
Hematuria, or the presence of red blood cells in the urine, may be microscopic (unable to be seen by the unaided eye) or macroscopic (visible with the unaided eye). More than three red blood cells per high power field (hpf) under the microscope indicates hematuria. It may also be glomerular (arising from the kidneys) or non-glomerular (arising from somewhere else along the urinary tract).
Glomerular Hematuria:
Non-Glomerular Hematuria:
Glomerular Hematuria:
- Inflammation of the glomeruli
- Injury to the glomeruli
- Leaking of red blood cells into the urine
- May also cause formation of red blood cell casts
- Often seen along with proteinuria
- Causes:
- IgA nephropathy
- Alport's disease (hereditary nephropathy)
- Benign familial hematuria
- Glomerulonephritis
- IgA nephropathy
Non-Glomerular Hematuria:
- UTI
- Benign prostatic hyperplasia
- Kidney stones
- Polyps
- Vigorous exercise
- Sickle cell disease
- Sickle cell trait
- Renal papillary necrosis
- Polycystic kidney disease
- Bladder cancer or tumor
- Prostate cancer or tumor
- Hypercalciuria
- Hyperuricosuria
- Medullary sponge kidney
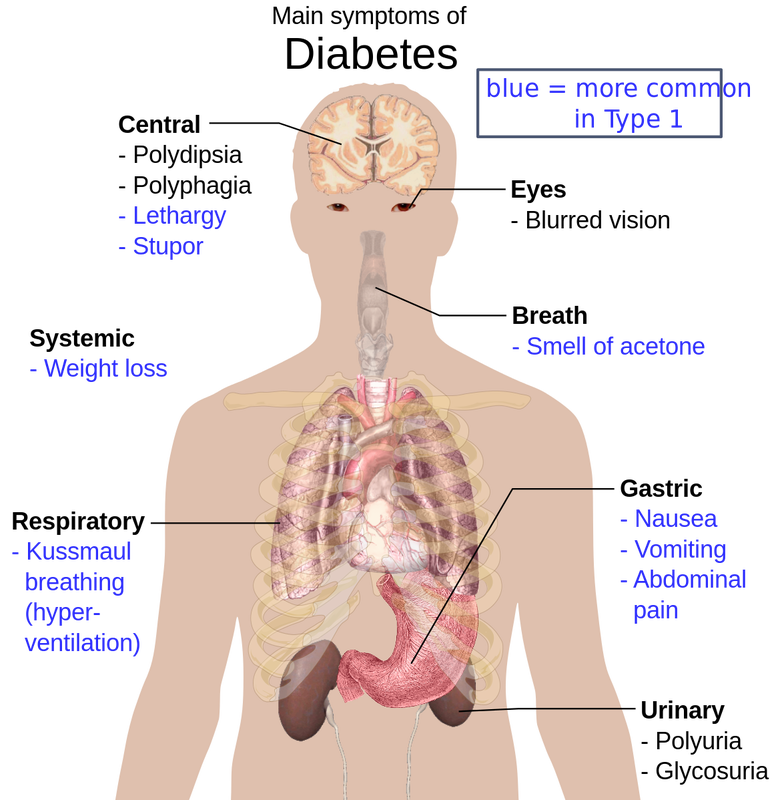
Diabetes, Type I: Insulin-Dependent and Type II: Diabetes Mellitus
- Diabetic nephropathy
- Renal changes that occur due to diabetes mellitus (glomerulosclerosis) which are irreversible
- Risk of increased morbidity and mortality
- Symptoms: urinary retention, nausea, high blood pressure, protein in urine, UTI, pyelonephritis, decreased GFR, elevated BUN level, increased cholesterol, protein and pus in urine, microalbumin
- Treatment: antihypertensives, diuretics, ACE inhibitor, fluids, low-protein/low-fat diet; long-term dialysis and eventual kidney transplant may be required
Glucoseuria: Symptom of Diabetes
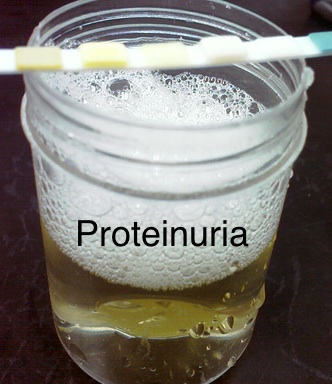
Proteinuria: Symptom of Diabetes
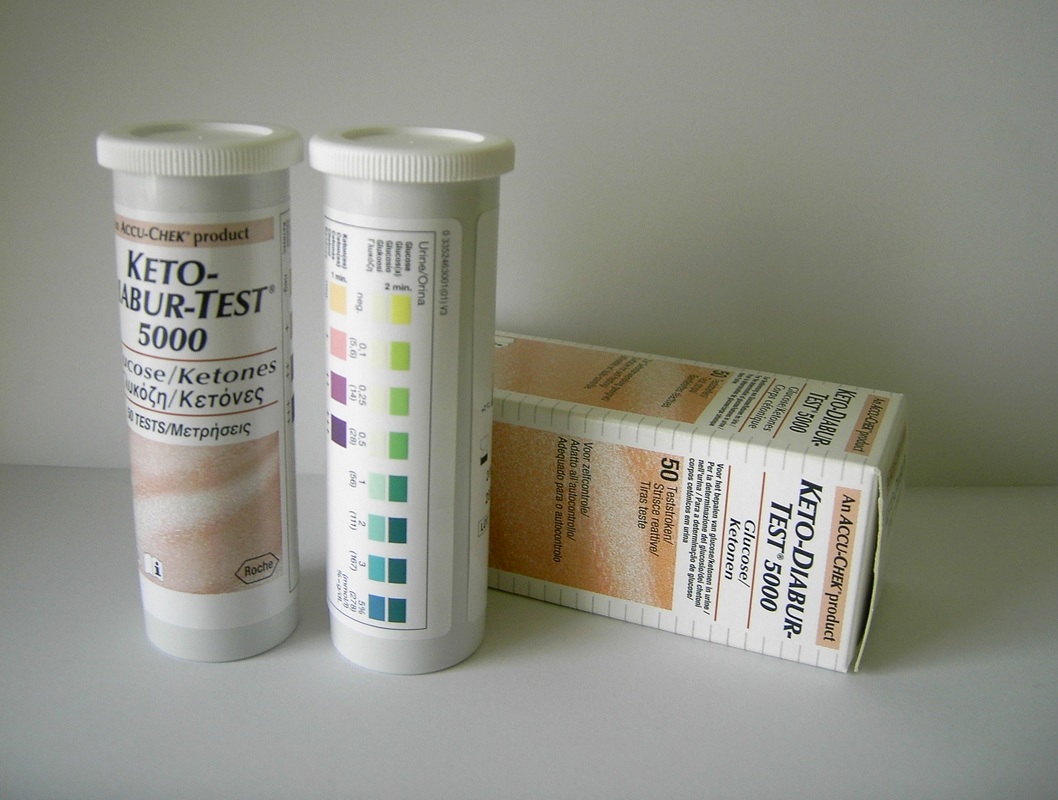
Ketone Acidosis/Ketonuria: Symptom of Diabetes
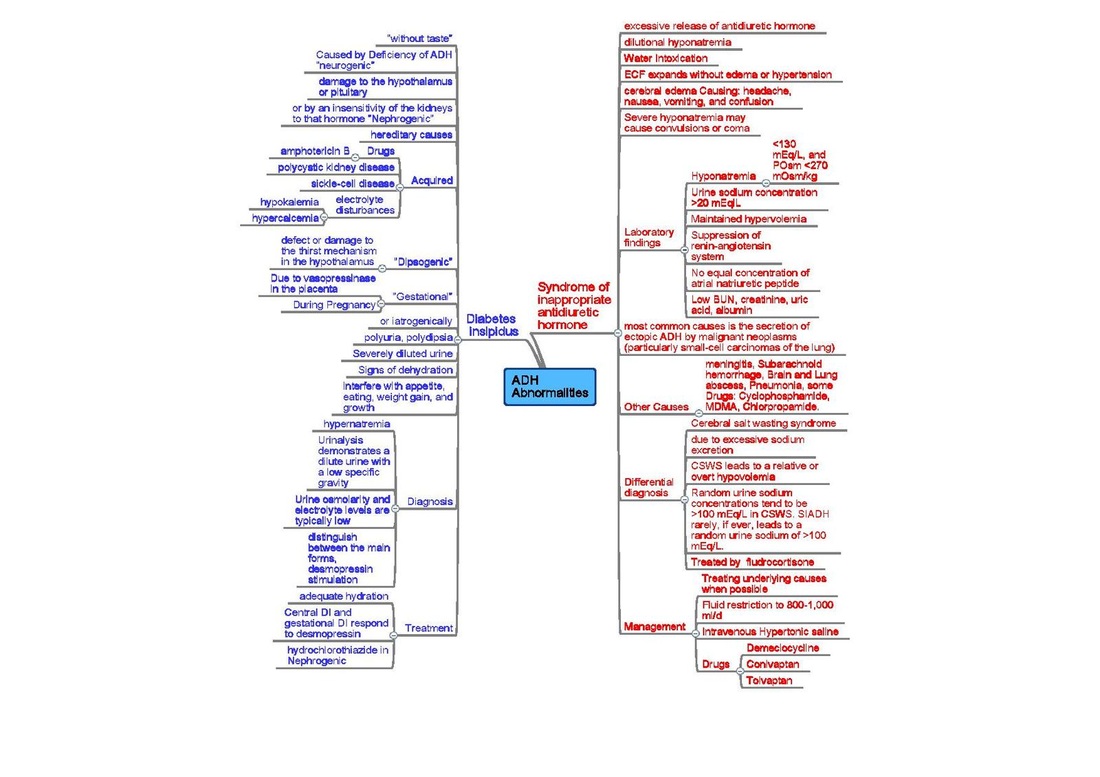
Diabetes Insipidis: Increased thirst, including at night, is a big symptom, along with dilute, clear urine
Nephritis
Nephrotic Syndrome (Nephrosis): Sodium and Water Retention, Puffiness, Casts, Proteinuria, Hematuria
- Nephrotic syndrome, also called nephrosis, is a disease affecting the basement membrane of the glomeruli of the kidneys
- This is often secondary to other primary renal diseases and systemic disorders
- Results in loss of huge amounts of protein (albumin) in the urine
- Decreased GFR occurs, resulting in severe water and sodium retention, edema and hypertension, as seen in the image below
- Also results in blood in the urine (hematuria), either microscopic or macroscopic
- Lipids are elevated
- Urinalysis shows fatty casts and sloughed off fat bodies as well
- Results in higher risk of infections
- Symptoms include lethargy, depression, loss of appetite, puffiness around the eyes, swelling of the ankles, pitting edema, weight gain, skin irritation, itching, headaches, side or pelvic pain
- Causes include glomerulonephritis, exposure to toxins or drugs, pregnancy, kidney transplant, metabolic disorders, diabetes mellitus, allergic reactions, infections
- Toxins:
- Acetaminophen
- Amphetamines
- Heroin
- Silicon
- Cyclosporin
- Certain antibiotics
- Lead
- Arsenic
- Mercury
- Pesticides
- Carbon tetrachloride
- Methanol
- Ethylene glycol (antifreeze)
- Ibuprofen and other nonsteroidal antiinflammatory drugs
- Radiographic contrast media
- Cleaning products
- Insecticides
- Organic solvents
- Treatment: treat underlying cause if possible, lower sodium and protein intake, diuretics, ACE inhibitors, corticosteroids, avoid certain drugs or toxins, monitor pregnancy or diabetes mellitus, allergic reactions
- May progress to end-stage renal disease
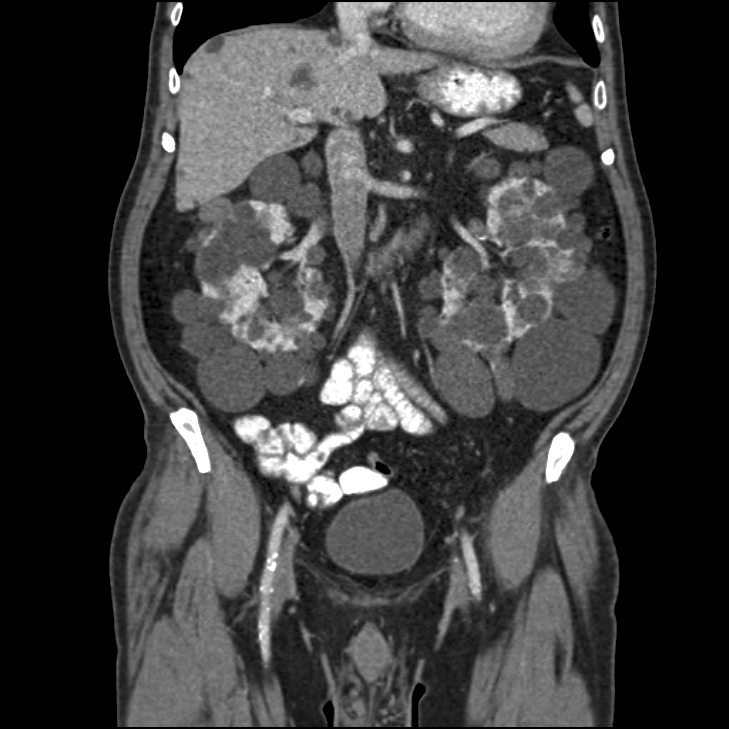
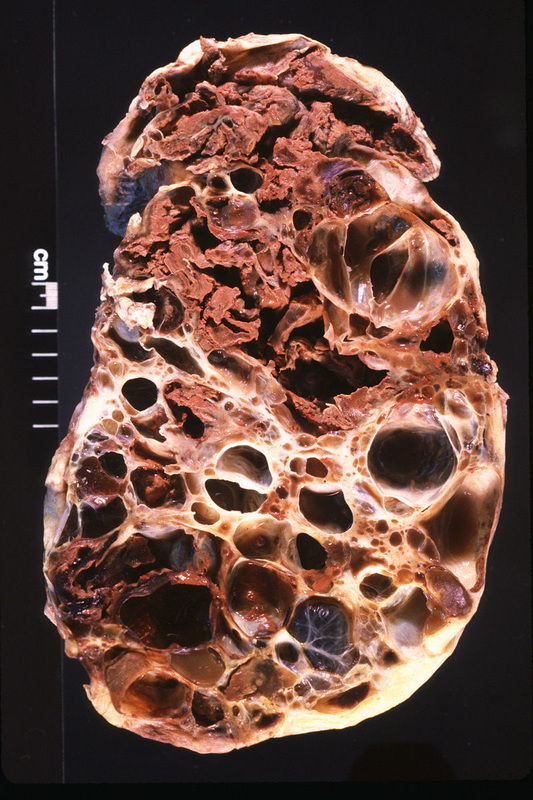
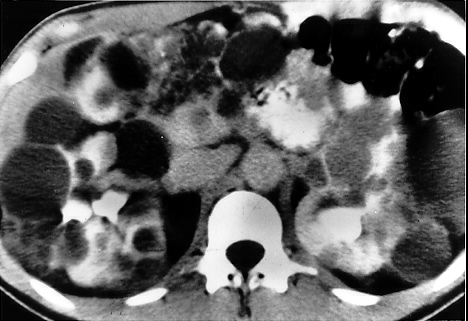
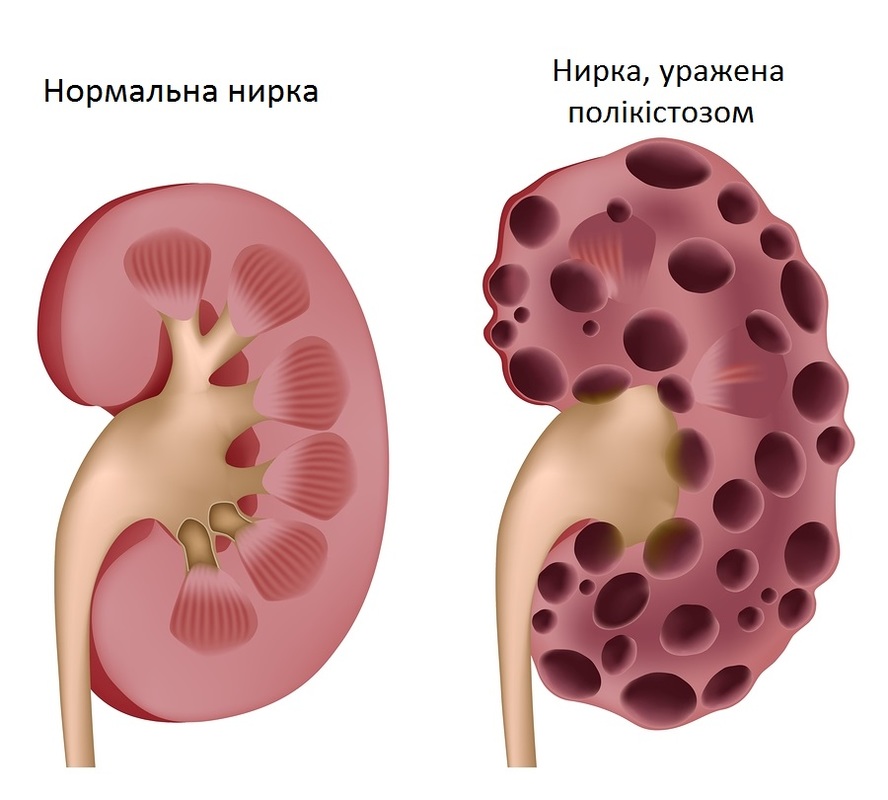
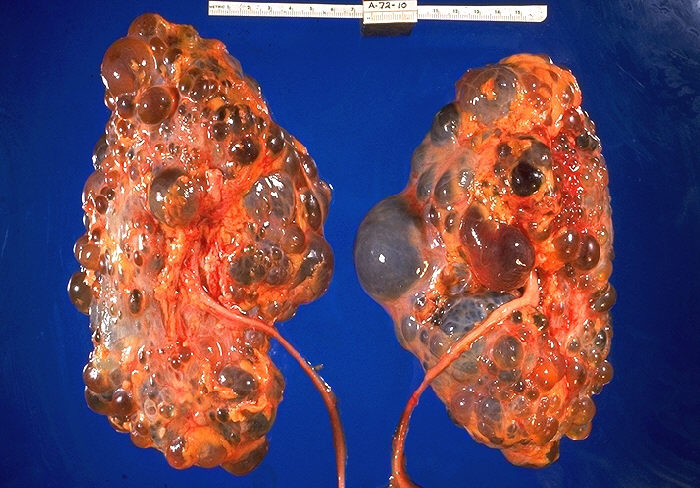
Polycystic Kidney Syndrome
- This is a slowly progressive disease, often familial and genetic
- Renal tissue is replaced with large cysts
- Affects both kidneys
- Kidneys become enlarged
- Causes loss of renal function and renal failure
- Symptoms: blood in urine, headache, edema, flank and pelvic pain
- Treatment: there is no cure; dialysis and transplant may prolong life; manage high BP and any UTIs
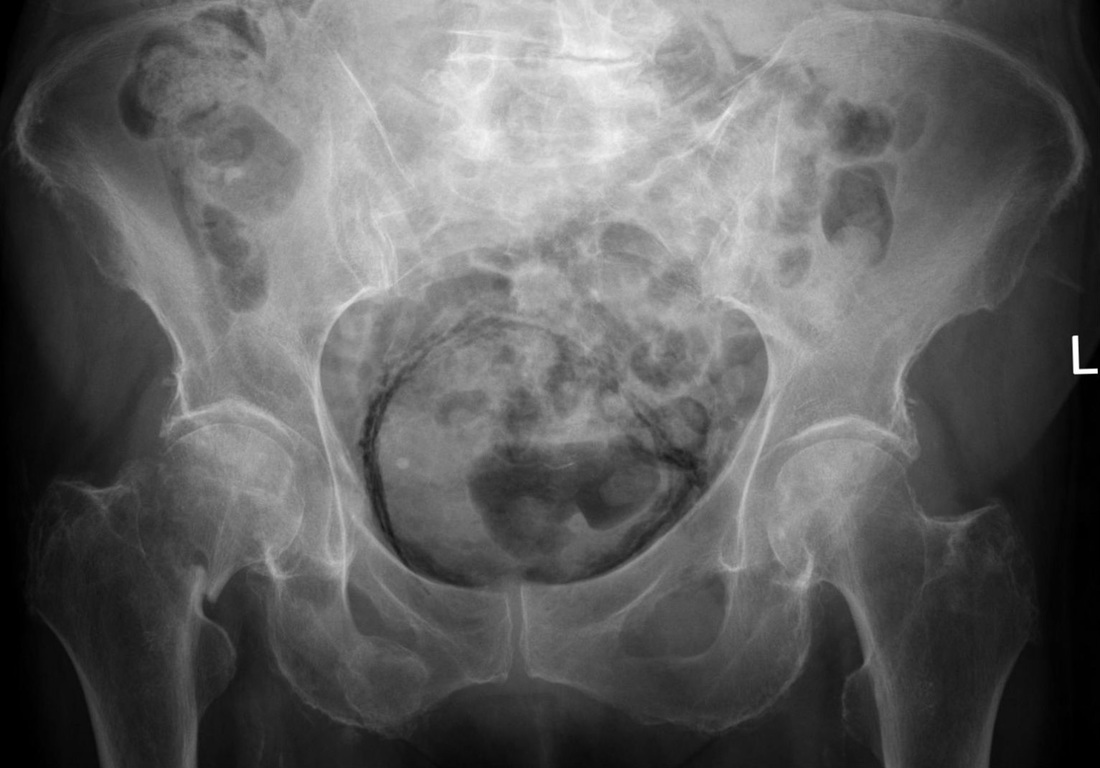
Bladder Stones
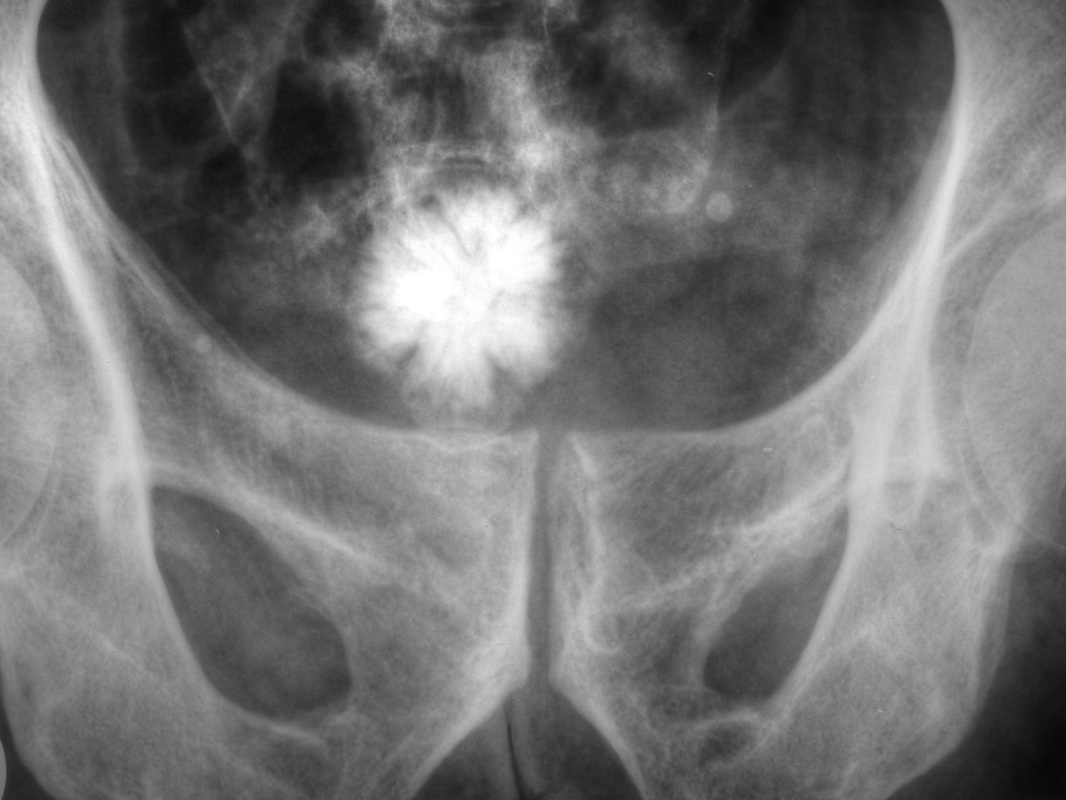
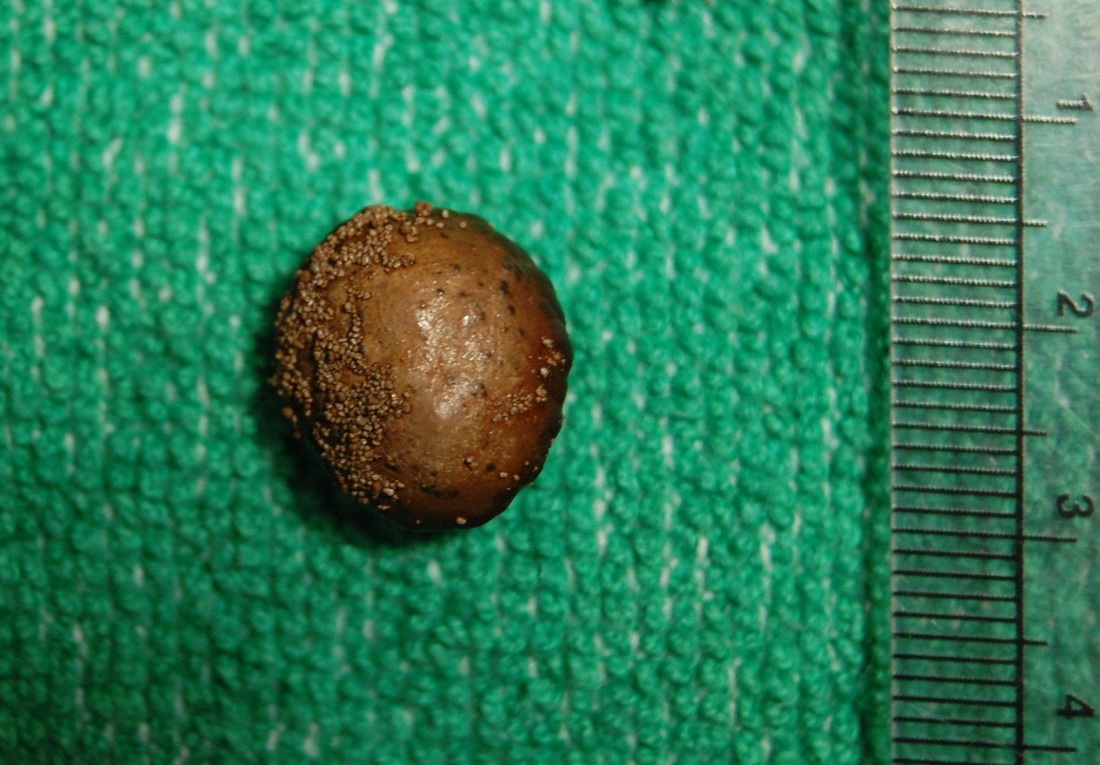
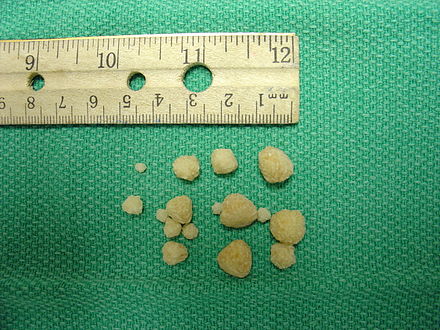
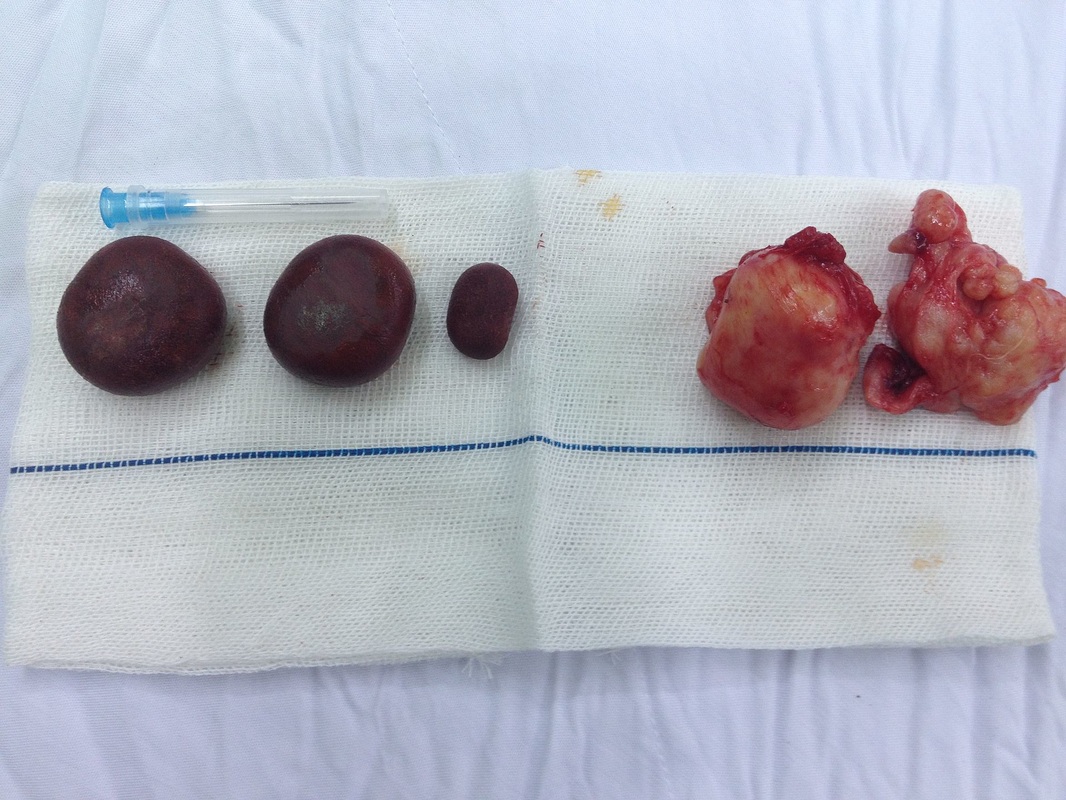
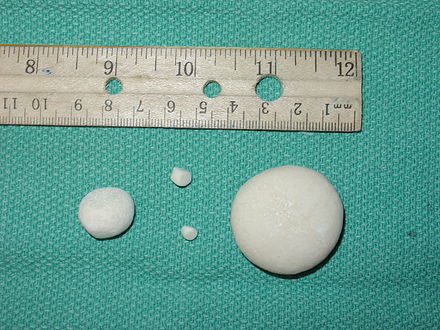
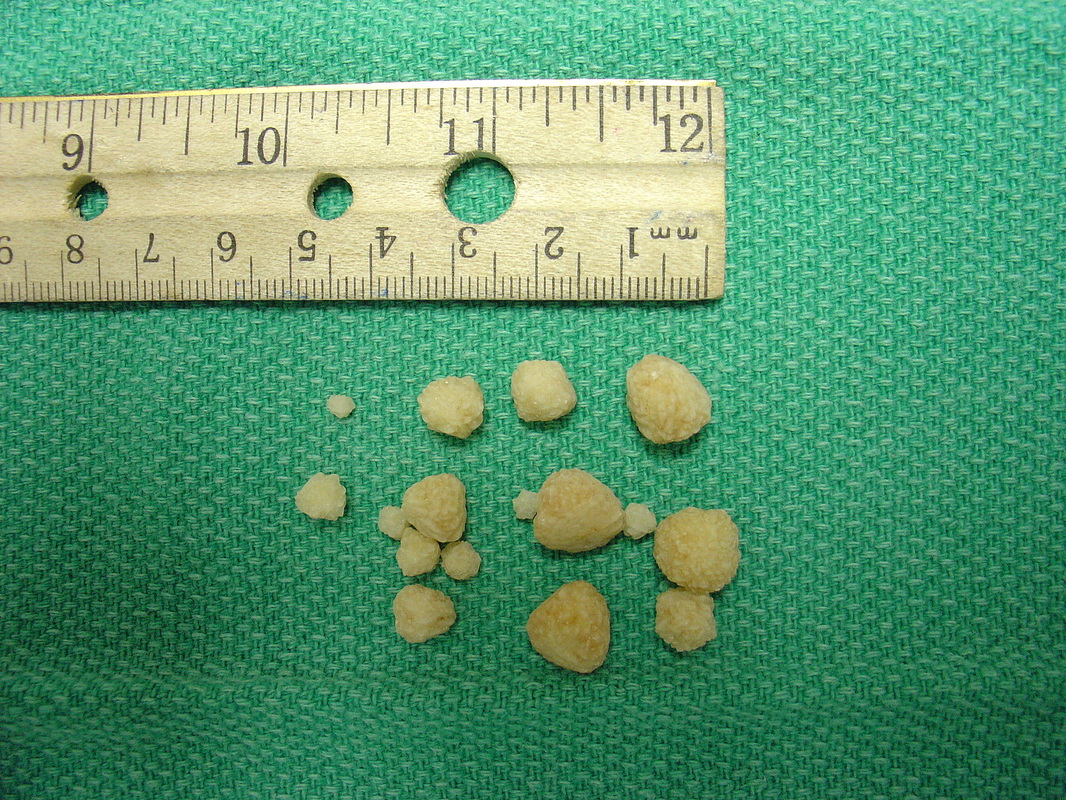
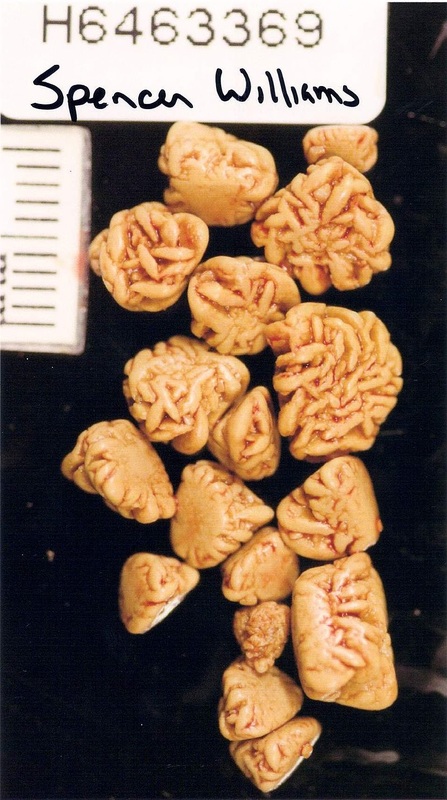
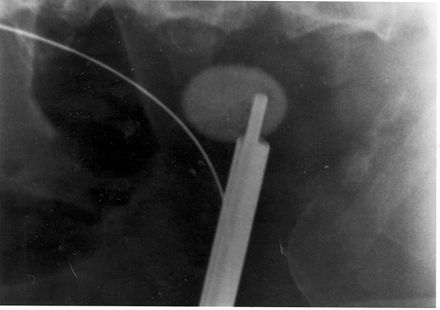
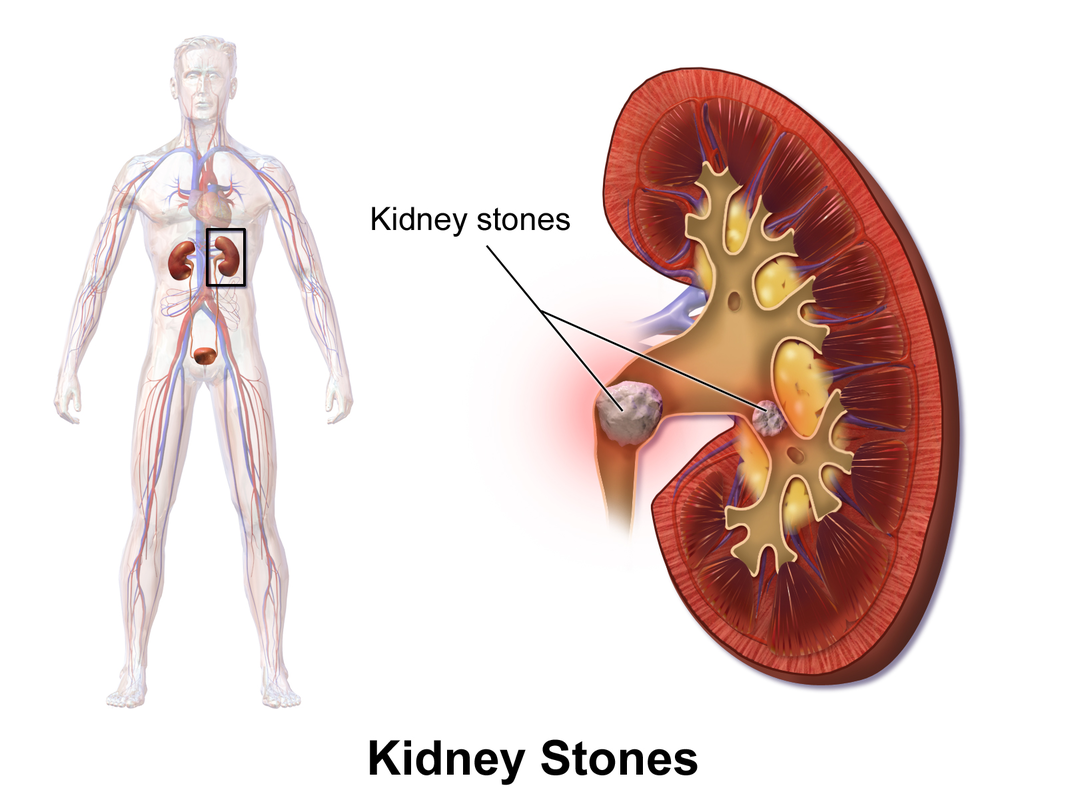
Renal Calculi: Kidney Stones/Ureter Stones
- Renal calculi: stones in the kidney or ureter or other areas of the urinary tract
- Caused by concentration of mineral salts, and there are a variety of different kinds
- Can occur on their own or in multiples and are various sizes and textures
- Smaller stones usually pass on their own, some even unnoticed
- Symptoms depend on size and type of stone and area of the urinary tract affected and if infection is also present, but do usually include renal colic (pain that comes and goes) on the side affected, urinary urgency, and sometimes blood in the urine; sometimes nausea and vomiting occurs, along with fever, chills and abdominal distension; sometimes hydronephrosis occurs
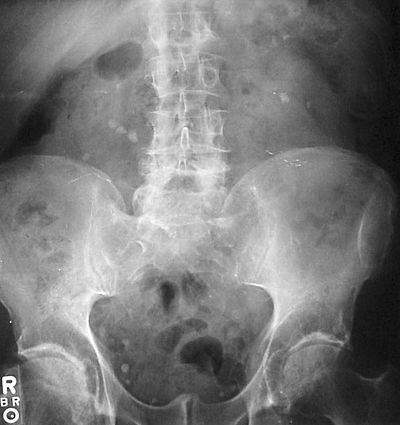
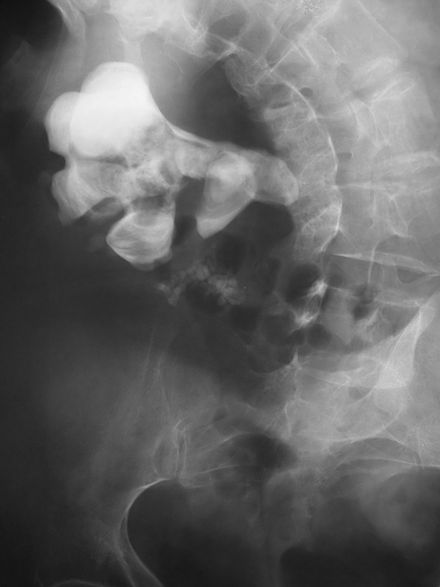
- Staghorn calculi: larger stones shaped like the renal pelvis where they are formed
- Causes: dehydration, excessive amount of calcium or uric acid present, immobilization, infection, urinary stasis, certain medications, gout, hyperparathyroidism, citric acid, foods containing oxalates, purines, or phosphorus
- Treatment: fluids, treat pain and infection, analgesics, catch the stone in a special sterile cup for evaluation, lithotripsy, surgery for larger ones or meds to dissolve them, stent placement
Stenosis and Reflux:
- Stricture or narrowing of the ureter or urethra, resulting in obstruction to flow of urine
Rhabdomyelitis
- Muscle breakdown and damage, resulting in blood in the urine
- Causes: congenital, medications, trauma, drug abuse, snake bites, electrical injury, heat stroke, heart attack, infections, lack of blood flow to a limb
Porphyriuria

- Genetic disorder resulting in blood in urine
Hereditary Galactosemia
- Genetic disorder that causes inability of sugars to be reduced and they spill over into the urine
- Genetic mutation in the gene that makes the enzyme galactose-1 phosphate uridylyltransferase (single missense mutation at exon 6)
- Genetic mutation in the gene that makes the enzyme galactose-1 phosphate uridylyltransferase (single missense mutation at exon 6)
- Inborn error of metabolism
- Inability to metabolize galactose, causing it to build up in tissues, resulting in failure to thrive, liver problems, cataracts, developmental delay, poor growth, and sometimes mental retardation
- Hereditary fructose intolerance is inability to metabolize fructose
- Lactose intolerance
- Glycogen storage diseases
- Usually detected in infants by the Clinitest or Benedict's Test for Reducing Sugars
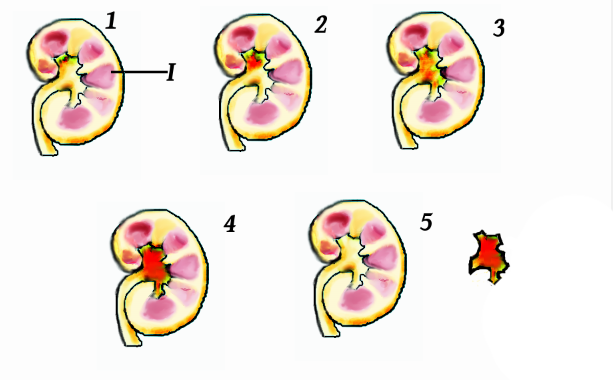
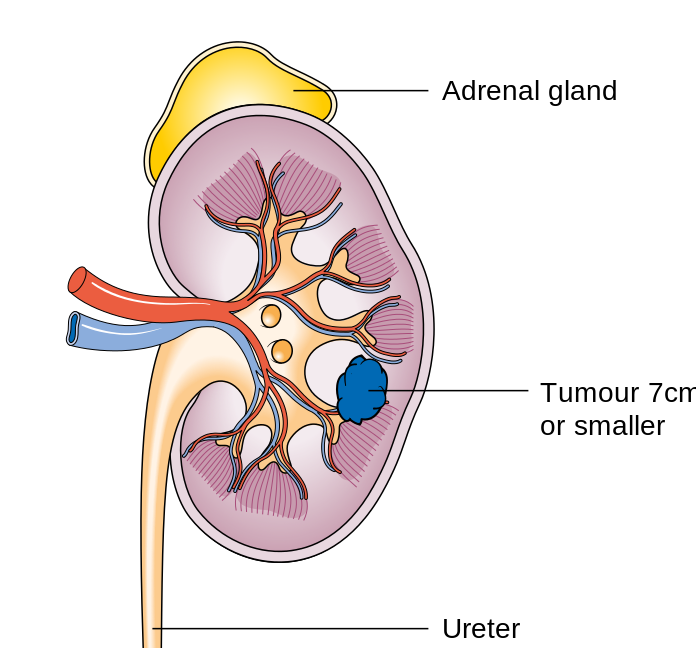
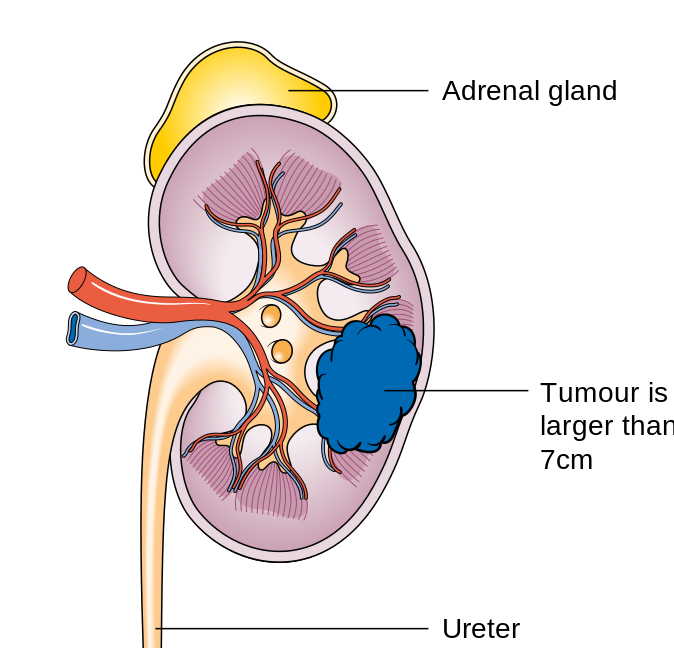
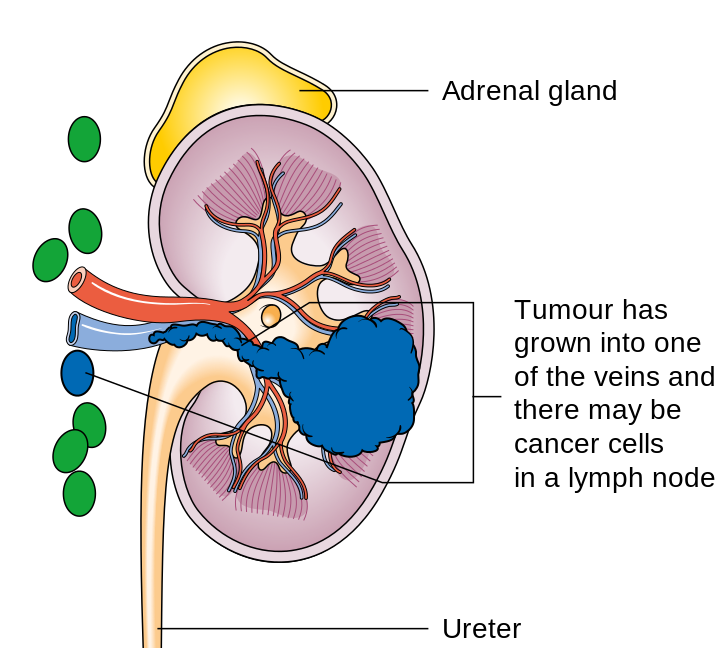
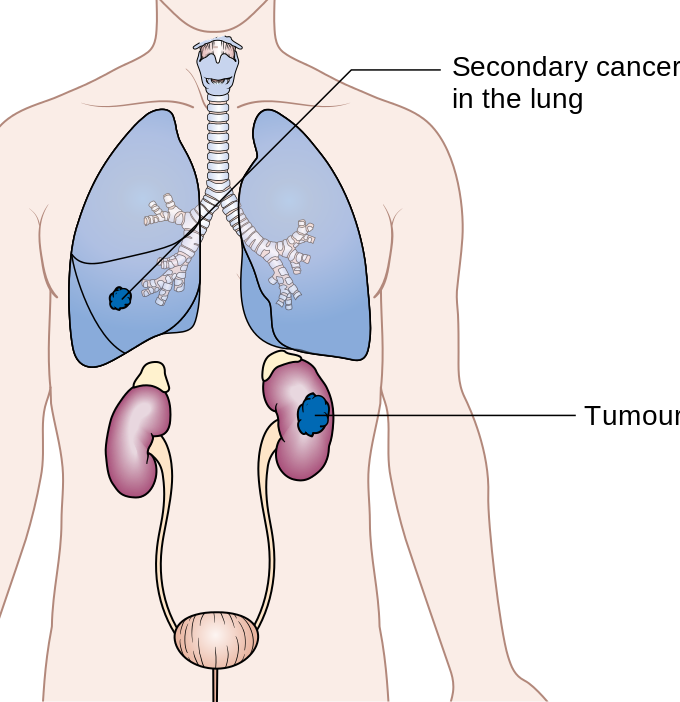
Kidney Cancer:
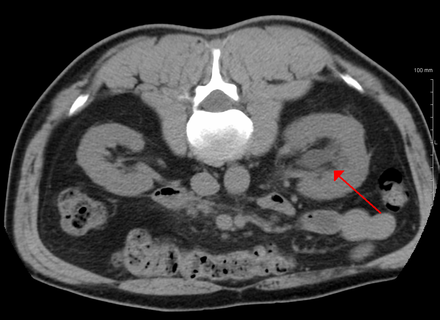
- Renal cell carcinoma: the most common primary tumor of the kidney
- Wilms' tumor: less common congenital tumor of childhood
- Renal pelvic cancer: less common
- One or more malignant tumors
- Mostly sporadic but some are familial (genetic)
- von Hippel-Lindau syndrome
- von Hippel-Lindau syndrome
- Symptoms: hematuria, abdominal mass, flank (side) pain, weight loss, loss of appetite, fever, hypercalcemia, hepatic dysfunction
- Risk factors: smoking, obesity, dialysis, acquired cystic kidney disease, exposure to chemicals or asbestos or cadmium
- Treatment: surgical removal of kidney or partial nephrectomy and chemotherapy
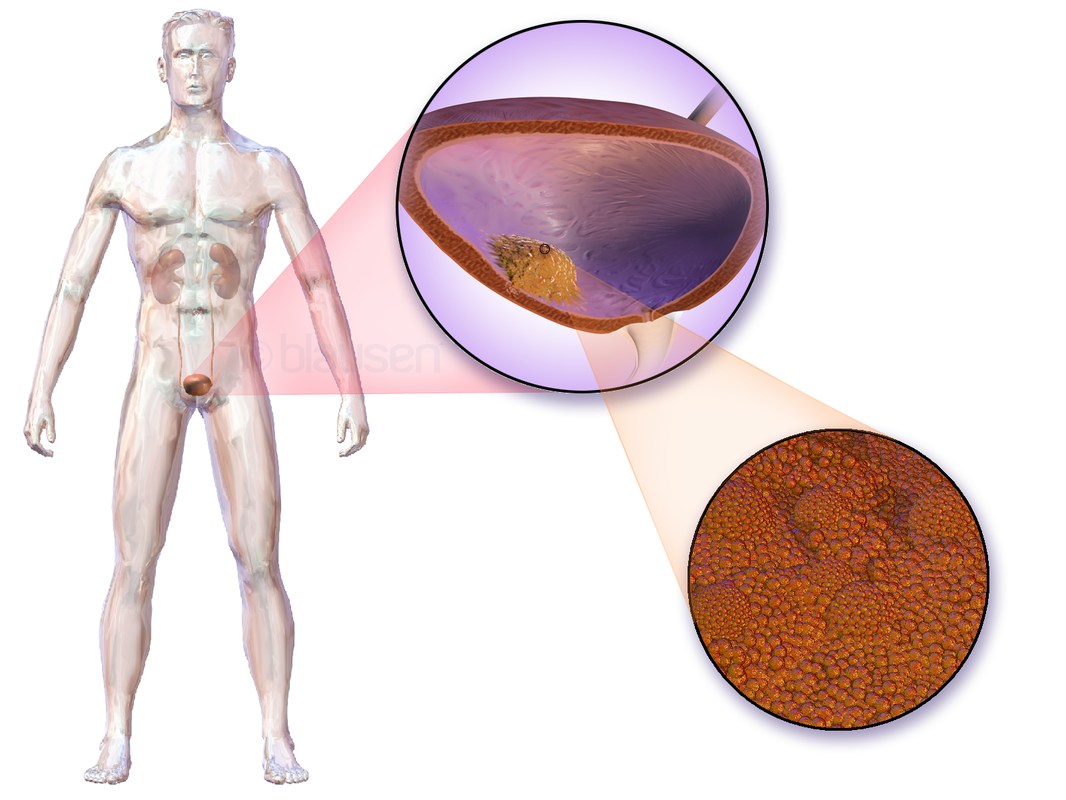
Bladder Cancer:
- Bladder neoplasms
- Usually occur in the transitional epithelium that lines the bladder, but some involve the squamous cells
- Symptoms: blood in urine, pain in flank or suprapubic region, dysuria, urgency, frequency, fatigue, weight loss, loss of appetite
- Cause: environmental exposures to chemicals or carcinogens, aniline dyes, diesel exhaust, smoking, prior schistosomas infection (parasite)
- Treatment: surgery, chemoradiotherapy if invasive
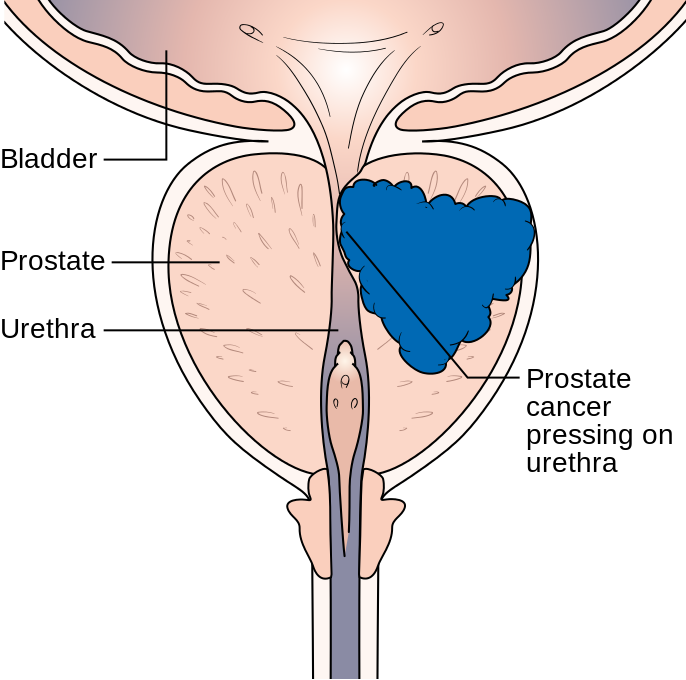
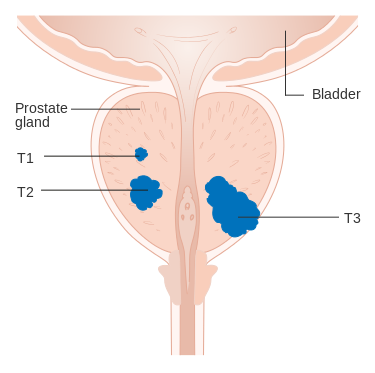
Prostate Cancer
- Develops in the prostate
- Most are slow-growing, but some are aggressive
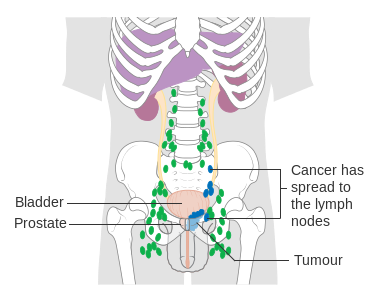
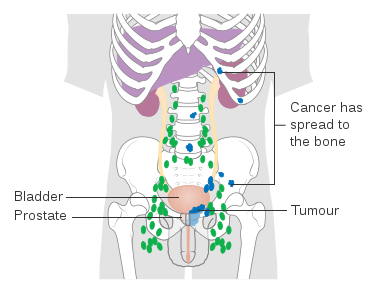
- If metastatic, may spread to the spinal vertebrae and lymph nodes
- In later stages, leads to difficulty urinating, blood in the urine, and back and pelvic pain, fatigue, anemia
- 99% of cases occur >50 years of age
- Genetics may have a link, as those with a sibling or parent with the disease or 2-3x more likely to get it themselves
- Diets high in red meat, processed meat and milk products may be linked
- Treatment: surgery, radiation, chemotherapy, drug therapy
Acute Renal Failure:
- ARF is sudden and severe
- Decreased renal function
- Considered an emergency
- Nitrogenous waste products build up in the blood very quickly, causing acute uremia
- Symptoms: sudden oliguria, gastrointestinal symptoms, headache, lethargy, dizziness or loss of consciousness, muscle weakness, heart palpitations, shortness of breath, excess bruising
- Causes: circulatory shock, heart failure, glomerulonephritis, stones, intrarenal damage), metabolic acidosis
- Very serious, affects other organs, can result in death
- Treatment: treat underlying cause first; monitor all body systems, dialysis, fluid intake/output balance, high carb/low protein diet, control of sodium/potassium intake, antihypertensives, diuretics, antibiotics
Chronic Renal Failure:
- CRF is gradual, progressive destruction and loss of nephrons
- Irreversible renal damage and loss of renal function
- Gradual onset of uremia
- Affects all body systems eventually
- Results in weakness, fatigue, lethargy, fluid retention and puffiness, edema, hypertension, uremic syndrome, heart palpitations, muscle weakness, shortness of breath, metabolic acidosis, ulcers, dry, brittle hair with thinning and hair loss, itching and dryness of skin, uremic frost, malaise
- Causes: glomerulonephritis, pyelonephritis, polycystic kidney disease, end stage of other renal diseases, chronic obstruction of urine due to tumors, cancers, or stones
- Treatment: dialysis or kidney transplant, diet modifications to control sodium/potassium, protein, diuretics, antihypertensives, antibiotics, calcitriol
- There is no cure
Hydronephrosis:
- Occurs when there is an obstruction in the urinary tract
- Causes dilation and swelling of the renal pelvis due to pressure from urine backup
- If this occurs consistently, long-term or is severe, will result in scarring and fibrous changes of the involved nephrons, with ultimate loss of function as well
- Usually chronic
- Typically does not result in pain or symptoms other than a vague backache or decreased urine output
- If infection occurs, patient will experience symptoms of pyelonephritis
- Treatment: treat the underlying cause
Neurogenic Bladder:
- Dysfunction of the bladder control
- Involves the signals or signal pathways involved in voiding
- Difficulty in emptying the bladder, as well as urinary incontinence
- Symptoms: hesitancy, decreased volume of urinary stream, retention, sensation of full bladder but unable to empty, persistent incontinence, spontaneous voiding of spurts of urine (reflex neurogenic bladder)
- Cause: often unknown; pregnancy; enlarged prostate; motor paralysis, damage to the brain, spinal cord, or nerves supplying the bladder due to trauma or disease, stroke (CVA), tumors, neuropathies, herniated lumbar disk, spinal cord trauma, polio, spinal cord lesion, myelomeningocele
- Treatment: no cure; drug therapy possible
Stress Incontinence:
- Uncontrollable leakage of urine (small amounts) during physical activity, exertion, exercise, laughing, sneezing, coughing, lifting, stretching, bending, running
- Cause: weakening of the pelvic floor muscles and urethra; usually results from the trauma of childbirth and hormones
- Treatment: Kegel exercises, estrogen therapy, drug therapy, surgical repair, collagen injections
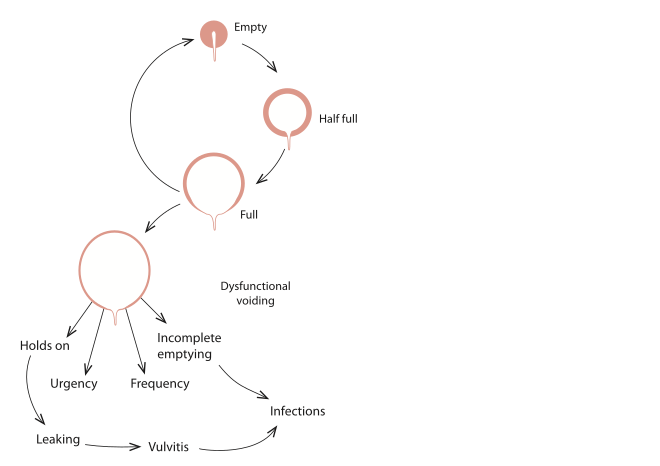
Overactive Bladder:
- A common ailment in today's society
- Urgency, incontinence, leakage of small amounts of urine, frequency, the need to urinate at night
- Treatment: Kegel exercises, PT for pelvic muscles, behavior therapy, drug therapy, biofeedback training of the sphincter
Urinary Incontinence:
- Reflex is overrun
- Normal reflex: initiates voluntary urination (micturition) when the bladder is full (distended)
- Sphincters of bladder and pelvic diaphragm relax
- Bladder muscles contract
- Bladder empties
- Sphincters of bladder and pelvic diaphragm relax
- Urinary incontinence is a partial or complete loss of voluntary bladder control
- Inability to retain the urine
- Elderly are most affected, as well as pregnant women and post-pregnancy (usually temporary)
- Enuresis: bedwetting
Medullary Sponge Kidney:
- Also called Cacchi-Ricci disease
- Congenital kidney disorder
- Characterized by formation of cysts in the collecting tubules of one or both kidneys
- At higher risk for kidney stones and urinary tract infections
- Benign
- May cause chronic renal (flank) pain in up to about 55% of patients
- Most incidences are asymptomatic
- May cause blood in the urine
- May lead to rare chronic kidney disease
- About
- Contact
- Introduction to Urinalysis
- Abnormal Urine Volumes
- Urine Specimen Types, Urine Collection, Specimen Preservation
- EXAMINATIONS OF THE URINE AND TESTS FOR
- ANATOMY AND PHYSIOLOGY OF THE URINARY TRACT
- Urine Chemistry and Pathophysiology
- PATHOPHYSIOLOGY OF DISEASES OF THE URINARY TRACT
- BACTERIAL INFECTIONS
- FUNGAL INFECTIONS
- PARASITE INFECTIONS
- VIRAL INFECTIONS
- Synovial and Joint Fluid
- Cerebral Spinal Fluid (CSF)
- Pericardial Fluid
- Peritoneal Fluid
- Pleural Fluid
- Amniotic Fluid
- References
- Automated Urinalysis